What is MRI Scanning?
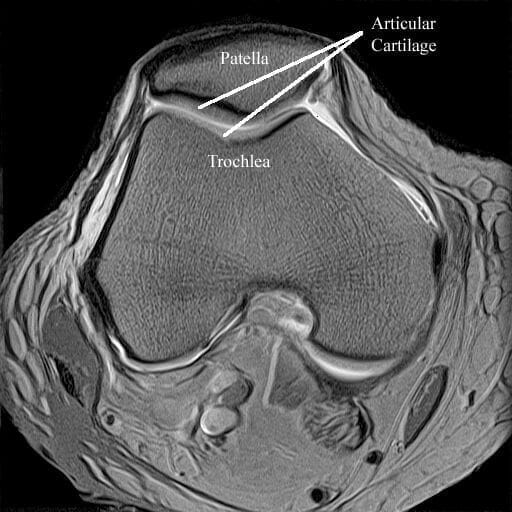
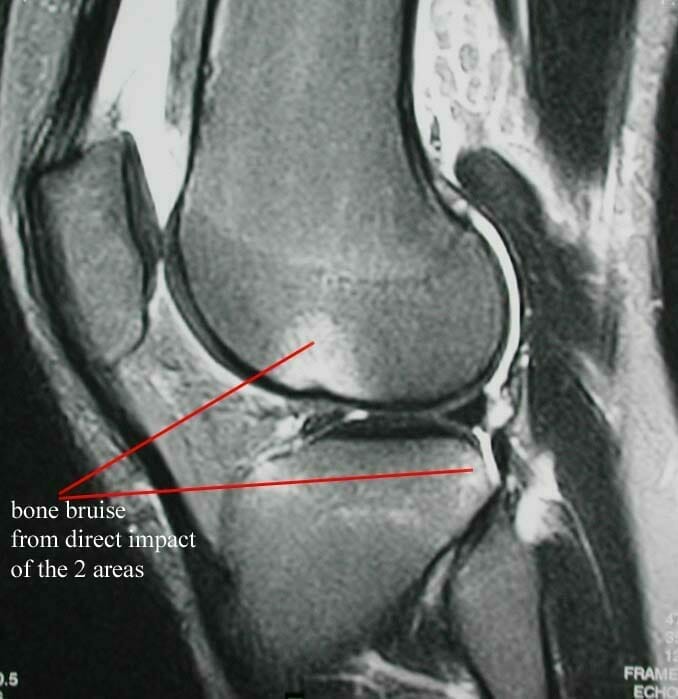
MRI scanning is a highly sensitive and specific non-invasive imaging modality of the knee. It works on the basis of magnetic field generation and release of magnetic energy from atoms within the tissues which have been energised and then de-energised. As they are de-energised they release magnetic radiation which is picked up by the MRI scanner. MRI scanning does not involve the use of any radiation. It is a very safe and non-invasive investigation. MRI scanning allows imaging in different planes and can also be used to generate three-dimensional models of the knee. Slices can be taken through the knee joint in planes at right angles to each other, as well as oblique planes to allow highly detailed imaging of particular components of the knee joint.
MRI scanning is very good at showing soft tissues, but is poorer at showing bone. It is commonly used to diagnose meniscal injuries, ligament injuries, articular cartilage damage, bone tumours, soft tissue tumours and can also show up other intra-articular abnormalities. MRI scanning is not 100% accurate. It will occasionally miss pathology and it will also occasionally show up abnormalities which are not clinically relevant. For example in the case of meniscal tears, MRI scanning is said to be between 90 and 95% accurate in detecting meniscal tears. Studies have been done which show that an examination by a well-trained and experienced knee surgeon is as accurate as MRI scanning in diagnosis meniscus injuries and tears. Because of the accuracy of MRI scanning, it is commonly used and in my view over used, for people with various complaints of knee pain. Clinically, prior to requesting an MRI scan, the surgeon should have a diagnosis or a list of diagnoses to confirm or refute. In most knee conditions, MRI scanning is not routinely required to make a diagnosis.
Am I Suitable for an MRI Scan?
There are situations in which patients cannot have MRI scans and this includes certain types of cardiac pacemakers, certain cardiac stents, cochlea implants, certain metallic foreign bodies for example maybe in the eye. The reason for this is that the powerful magnetic fields that are generated can cause damage by making the foreign bodies move, or by stopping other implanted devices from working. Having a joint replacement in your body does not prevent you from having an MRI scan. Other relative contraindications include gross obesity when it is physically impossible to fit in the scanner. Very young children need to be given a general anaesthetic, as in order to have an MRI scan, the patient must lie absolutely still. People who are claustrophobic may not like going into an MRI scanner and certain stages of pregnancy may be contra-indicated for MRI scanning.
MRI scanning requires experienced reporting by musculoskeletal radiologists in addition to reviewing the films myself. I am fortunate to work with highly trained musculoskeletal radiologists who I work with routinely to report my musculoskeletal imaging.
An area where MRI scanning is now starting to develop specifically is in the area of imaging of articular cartilage which has great relevance for articular cartilage injury, such as chondral and osteochondral defects, as well as cartilage transplantation procedures. Current MRI scanners do not have the power to provide the resolution that is always needed for good articular cartilage imaging. However, I am fortunate to have the ability to access one of the few 3 Tesla (the higher the Tesla value of an MRI scanner, the more power it is and the greater resolution that can be obtained from it. Most MRI scanners and 1-1.5 Tesla), scanners with which we are currently devising research protocols. We are however, using it in a clinical situation for articular cartilage imaging, where it is proving to be highly valuable.
Dynamic MR imaging can be used to assess patella tracking during active flexion.
MRI scanning has emerged as the imaging modality of choice, for evaluation of the musculo-skeletal system. MRI provides non-invasive multiplanar assessment of bones and joints with exquisite anatomical detail and superior spatial resolution and without exposing the patient to ionising radiation. MRI detects very subtle changes and differences in tissue characteristics, allowing earlier and more specific diagnosis of pathological processes than any other imaging modality.
How does MRI Work?
All diagnostic MRIs based on imaging hydrogen atoms (protons) contained in fat and water molecules. When placed within a magnetic field, the hydrogen nuclei, being themselves small magnets, will align in the direction of the field, just as a compass does in the Earth’s much weaker magnetic field. The equilibrium that is established is disturbed by knocking these small anatomic magnets out of alignment by specific radio frequency pulses. As these protons re-establish equilibrium, when the radio frequency pulse is switched off, they will emit a radio frequency signal that is detected by a receiving antenna (surface coil) and analysed by the computer to generate an image. The time required for these hydrogen nuclei to regain an equilibrium state can be measured in terms of what is called a relaxation time. In the case of MRI, there are 2 relaxation times: T1, the longitudinal relaxation time and T2, the transverse relaxation time. The T1 and T2 relaxation times are intrinsic parameters specific to a given tissue. The primary operated dependent extrinsic parameter used in clinic MRI are the repetition time (time between successive radio frequency pulses) and the echo time (the time between the radio frequency pulse and the sampling of the emitted tissue signals). These intrinsic and extrinsic parameters will directly affect the spin echo signal intensity of different types of tissues.
Different tissues in the body behave in a reproducible manner on specific pulses sequences and knowledge of these characteristics is helpful for the detection of pathological processes. For example fatty tissue is bright (hyperintense) on T1 weighted images and less intense on T2 weighted images; hemopoietic bone marrow is lower in signal intensity on T1 and T2 weighted images than is fatty marrow owing to the level of fat content. Water is bright on T2 weighted images and dark on T1 weighted images. Because pathological processes (tumour, infection, concussion) are typically associated with increased water content, abnormalities usually appear hyper-intense to the adjacent tissues on T2 weighted images and lower in signal intensity on T1 weighted images.

Make An Enquiry
Or contact us directly
[email protected]
0161 445 4988
